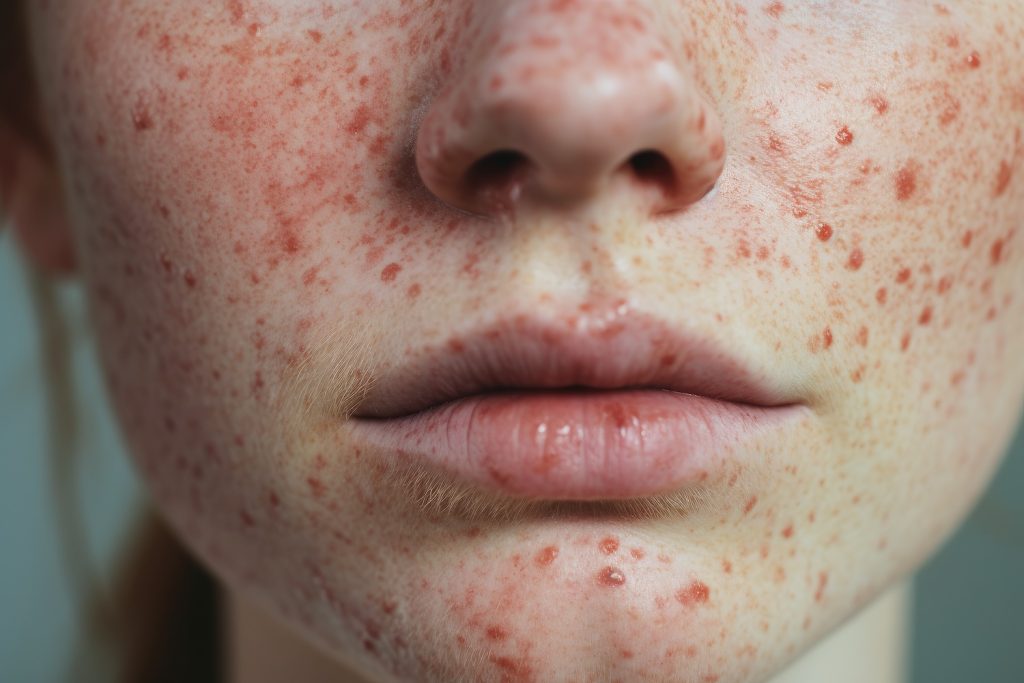
Have you ever heard of fungal acne? It’s not your typical acne. If you’ve been struggling with small, itchy pimples that don’t seem to go away, it could be fungal acne, which is different from the usual acne most people know. It’s caused by an overgrowth of yeast, not bacteria.
Imagine Sarah, a 25-year-old who noticed small red bumps on her forehead. They were itchy and seemed different from the usual acne she had experienced as a teenager. After trying various acne treatments with no luck, she learned that she had fungal acne. This story isn’t unique. Many, like Sarah, mistake this for regular acne and don’t know how to treat fungal acne.
Fungal acne, or Malassezia folliculitis, is a skin condition often mistaken for regular acne or acne vulgaris. This type of acne is caused by an overgrowth of yeast in the hair follicles (Pityrosporum folliculitis). This yeast is naturally present on everyone’s skin and is part of your regular skin flora, but when it grows too much, it causes problems.
The accumulation of dead skin cells can contribute to fungal acne as this arises from specific factors that encourage the overgrowth of yeast on the skin, and certain conditions can disrupt the balance, leading to an overgrowth.
Athletes and individuals who lead active lifestyles are more prone to developing fungal acne due to frequent sweating, their skin rubbing often and wearing tight clothes. This sweat can create a favourable environment for yeast growth. Similarly, teens and young adults are at a higher risk, as hormonal changes during these years often increase oil production in the skin, contributing to the conditions that favour the development of fungal acne.
Unlike regular acne, fungal acne often comes in various sizes and shapes, where the pimples are generally small, red, and similar sizes. If you’ve been treating your skin with typical acne products and see no improvement, it might be because you’re dealing with fungal acne.
A distinct feature of a fungal infection is itchiness and burning.
Fungal acne often shows up in areas where sweat accumulates, like:
Here’s a simple way to think about it: If your skin problems worsen with sweat and oil, it might be fungal acne. Most acne treatments are designed to reduce bacteria and unclog pores. Since fungal acne is yeast-based, these ineffective treatments can sometimes worsen the condition. Remember, fungal acne isn’t about poor hygiene. It’s your skin’s reaction to an imbalance of the natural yeast.
A fungal acne diagnosis typically involves a thorough examination of the skin and may include tests to confirm the presence of an overgrowth of yeast. There are various ways to treat fungal acne.
Antifungal creams are a frontline treatment for fungal acne. Products like Trimovate cream, Fucibet cream, and Daktacort cream effectively combat the yeast. These creams are applied directly to the affected areas and can quickly reduce symptoms.
Antifungal shampoos like Nizoral can be beneficial for treating larger body areas. These shampoos contain ketoconazole, an ingredient effective against the yeast causing fungal acne. You can use them as a body wash on the affected areas.
When topical treatments don’t provide sufficient relief, a GP or pharmacist might recommend oral antifungal medications like Fluconazole. These medications are potent and address the condition internally.
Besides specific antifungal creams, other topical treatments like azelaic acid can help manage fungal acne. They help balance yeast growth on the skin and prevent flare-ups.
Consult a GP or pharmacist before starting any treatment, as they can offer personalised advice and recommend the most suitable treatment for your condition.
Fungal acne and regular acne might look similar, but they have distinct differences in several aspects:
Preventing fungal acne breakouts involves a combination of good skincare routines and lifestyle choices, so keep your skin clean and dry. Regularly wash areas prone to fungal acne, especially after sweating and choose non-comedogenic skincare products that won’t clog pores.
Wearing loose, breathable clothing can also help, as tight clothes trap moisture and create a livable environment for yeast growth. Maintaining cleanliness in your living environment is essential, too. Change bed sheets and towels frequently, especially if you live in a humid climate.
Pay attention to your diet as well. Balancing your consumption of sweets and foods high in carbohydrates can be beneficial, as fungi and yeast thrive on these nutrients. This dietary adjustment might help in slowing down the growth of fungal infections.
Regular exercise and stress management also play a role. Physical activity promotes healthy blood flow, while stress management techniques like meditation can improve your overall well-being, impacting your skin positively.
If you’re struggling with fungal acne or other skin concerns, Click2Pharmacy’s Online Acne Treatment Clinic can help. We offer personalised advice and treatment plans, and our team of licensed professionals understand the unique challenges of skin conditions like fungal acne.
You can reach out to us for an online consultation. Whether you need advice on treatment options, prescription services, or just someone to guide you through your skincare journey, our pharmacists at Click2Pharmacy are there to assist you.
Don’t let fungal acne affect your life. Contact us today for expert care and support in managing your skin health.
Get 10% Off Your First Order
Sign up to receive special offers via email and get 10% off your first order*
By opting in to marketing, you agree to our terms & conditions and privacy policy.